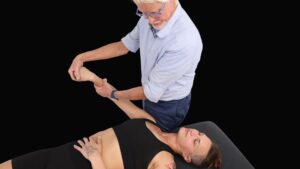
Introduction
Year-round sports are a way of life for many and involve people across all age groups. From elite professionals and athletes with an avid interest to casual participants and folks who simply want to stay fit, all are at risk for cumulative trauma disorders (CTDs). CTDs are generally described as tissue damage resulting from repetitive demand over the course of time. The term refers to a vast array of diagnoses stemming from occupational, recreational, and habitual activities.
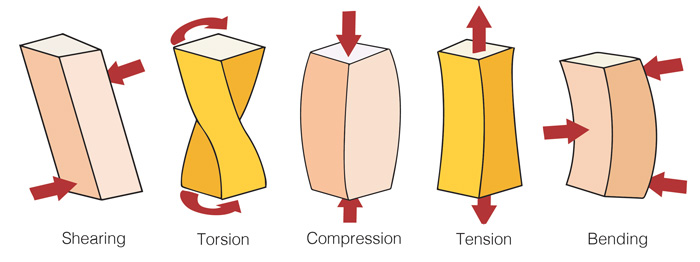
It was established more than 100 years ago that biological tissues adapt to the level of stress placed upon them.1 Today, researchers such as Lorimer Moseley call that process “bioplasticity.” All kinds of injuries, such as tennis elbow, runner’s knee, and “pulled” hamstrings, can occur due to overuse. Shear, torsion, compression, tension, and bending are the injury mechanisms we tend to see in such cases (Image 1). Mechanical strain in tendons, ligaments, nerves, and other connective tissues results in fatigue and may lead to body-wide compensations, reactive spasm, and — if the brain senses threat — pain.
Is It a Muscle Imbalance Problem?
It makes sense that weak muscles become strained more easily than strong muscles if the athletic activity is performed with poor motor control. Muscles that are habitually used in either stretched or shortened positions are weaker and more prone to injury. Try this exercise: Make a fist with your wrist straight. Now flex your wrist to stretch the forearm extensor muscles, and then extend to shorten the same muscles. Notice how your wrist weakens in this flexed position. This even applies to the large back muscles, but it is particularly problematic in muscles that cross two joints, such as the hamstrings (the hip and knee), the calf (the knee and ankle), and the quadriceps (the hip and knee).
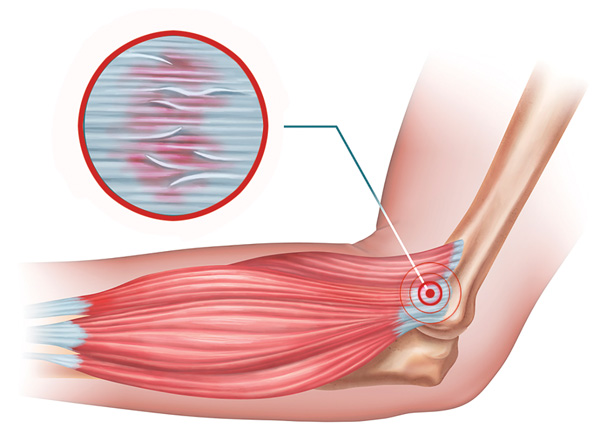
CTDs are commonly seen in tendons. As a tendon is loaded and the strain increases, there is microscopic tissue deformation, and some fibers begin to fail (Image 2). Ultimately, macroscopic tendon failure occurs. It’s important to remember that tendon degeneration is not necessarily the result of inflammation. Histologic findings in athletes with overuse tendon injuries such as tennis elbow do not show signs of inflammation (i.e., there are no inflammatory cells present in surgical specimens).2 While tendinitis is an acutely inflamed swollen tendon without microscopic tendon damage, tendinosis is a chronically damaged tendon with disorganized fibers and a hard, thickened, scarred, and rubbery appearance.
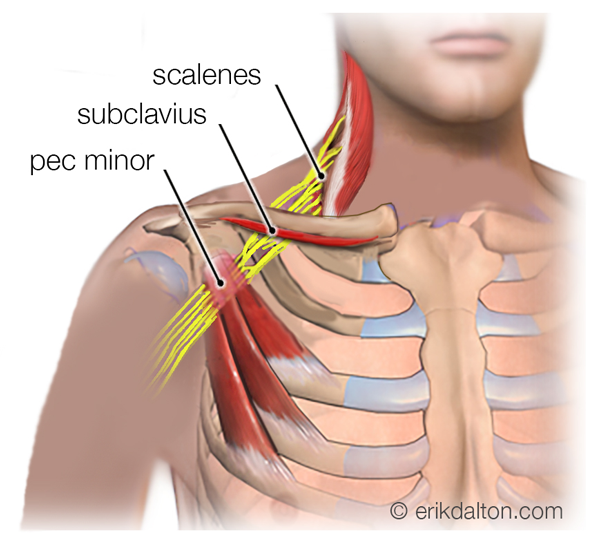
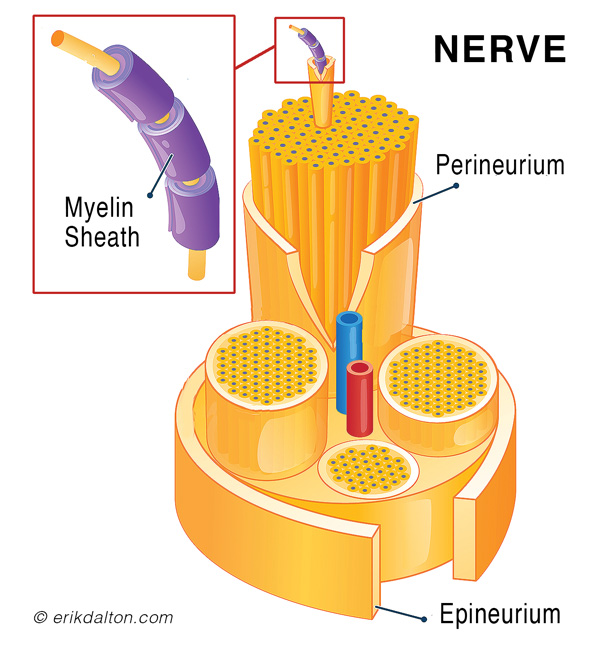
In disorders such as piriformis and thoracic outlet syndromes, nerve tissues are at particular risk for ischemic injury (Image 3). Compression, nerve entrapment, and eventual loss of blood supply lead to characteristic changes in the nerve itself. The length of time a tissue can survive oxygen deprivation varies, but all ischemic tissue will eventually become necrotic under such circumstances. The timeline generally begins with subperineurial edema, followed by thickening of the perineurium, stiffening of the epineurium, thinning of the peripheral myelin sheath, and — as the nerve breaks down — axonal degeneration (Image 4). Restoration of blood and oxygen supply via massage often minimizes damage, but not always. It primarily depends on the type of structure causing the compression (bone, muscle, intervertebral disc, etc.) and the degree of load on the nerve.
The causes of microtraumatic overuse injuries are often less obvious compared to the macrotrauma of an acute injury. During the early stages of a CTD, there is little or no pain and the person might unknowingly continue to place pressure on the injured area. As a result, the involved tissue doesn’t have the necessary time to heal. Repetitively applied stresses that are below the tensile limit of the injured tissue typically result in positive remodeling, but not without adequate rest, retraining, and skilled bodywork.
What Role Does the Brain Play in CTDs?
The SAID principle — an acronym for Specific Adaptation to Imposed Demands — is a classic sports medicine term describing how physical adaptations develop when the body is placed under stress, thereby allowing us to better handle future stressors.
Stated simply, the body gets better at doing whatever it does regularly.
Unfortunately, as our bodies get better and better at seemingly “looking after us,” peripheral nerves can become hyperexcited and begin conveying danger-signaling messages. As the area becomes more sensitized, brain cells that are triggering the pain are on high alert.
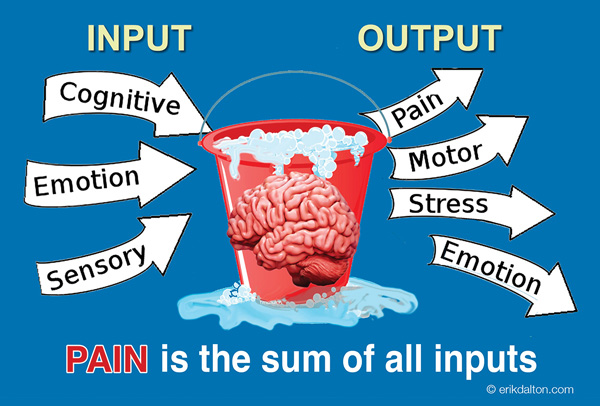
Image 5 shows how increased cognitive, emotional, and sensory input can accumulate in the brain. Any additional input from a chronic or acute injury can cause these protective coping systems to overflow into things such as reactive muscle guarding, stress, and pain. Our job as therapist is to help lower the threat level in the stress bucket through good bodywork and by coaching the client on new ways to move, think, and behave.
Immediate treatment should include training modifications, graded exposure stretching of injured connective tissues, and stabilization of weakened areas. For long-term improvement, biomechanical alignment problems also need to be addressed. A comprehensive approach to rehabilitation of CTDs provides the best hope for many years of pain-free recreational enjoyment.
References
- Wolff, J. (1986). The law of bone remodeling (P. Maquet & R. Furlong, Trans.). Springer-Verlag. (Original work published 1892)
- Boyer, M.I., & Hastings, H. (1999). Lateral tennis elbow: Is there any science out there? Journal of Shoulder and Elbow Surgeryu, 8(5): 481–491.
On sale this week only!
Save 25% off the Art of MAT course!
Take an inside look at Myoskeletal Alignment Techniques in action. Follow along with Erik Dalton as he uses MAT techniques to treat real people with real problems. Click the button below for more information and to purchase the course for CE hours and a certificate of completion to display in your office. BONUS: When you purchase the home study course, receive the eCourse for free!
Save 25% this week only. Offer expires May 31st!