The following is an excerpt written by Adjo Zorn and Kai Hodeck from chapter #7 of Erik Dalton’s book, Dynamic Body: Exploring Form Expanding Function, which features guest contributions from some of the leading thought leaders and practitioners in the massage profession. The rest of the chapter can be read in the Dynamic Body textbook, available as part of the Dynamic Lower Body home study course or as a standalone purchase.
Questioning Generally Accepted Views About The Nature Of The Most Common Tissue In The Human Body
We daresay there is a lot of confusion in the medical world regarding the nomenclature and characteristics of tight connective tissue. This confusion can, unfortunately, lead to confusion in discussions regarding how tendons, fascia, and the like work together during human walking. Therefore, we would like to clarify a few foundational concepts.
First:
We would like to clear up the misconception regarding the elastic properties of collagen and elastin. If a person thinks steel is hard and rubber is elastic, we have to remind him, “what cannot bend will break.” He does not realize that steel is strong because it is elastically yielding. The yielding motion is so small that it escapes observation. Early anatomists were of the same sort, and their erroneous thinking is still alive today.
Henry Gray’s classic 1918 publication Anatomy of the Human Body states, “Tendons are devoid of elasticity.” These early anatomists distinguished between “elastin” and “collagen” fibers in the connective tissue. Colla is the Greek word for glue and a misleading denotation. Today, the elasticity of collagenous tissue is demonstrated beyond any doubt, not only by hopping kangaroos, but also in laboratories showing the properties of tendons, ligaments, and fascia in various mammals.
However, many of the most respectable physiologists still write about “elastic and collagenous fibers,” implicitly suggesting that collagen fibers are not elastic. They should at least use the correct – though still unfortunate – term “elastin and collagen fibers.” Even worse, practitioners of both conventional and complementary medicine often speak blithely about “non-elastic collagen.” Next time a person tells you how non-elastic collagen is, you might want to show him Christopher Anderson’s video, featuring the projection of chameleon tongues.1
The difference between elastin and collagen is not about being more or less elastic – both are of the elastic kind – but rather that elastin and collagen have different quantities of elastic stiffness. (Young’s modulus is used to quantify the stiffness of an elastic material.) Collagen is approximately 100 times stiffer than elastin, meaning it can store the same amount of energy while stretching only one-hundredth the amount. A 1957 text written by Henry Bull, a professor of physiological chemistry, states: “Since collagen fibers are not much extensible, their elastic properties, so far as biology is concerned, are of limited interest.”2 In our opinion, this statement is nonsense.
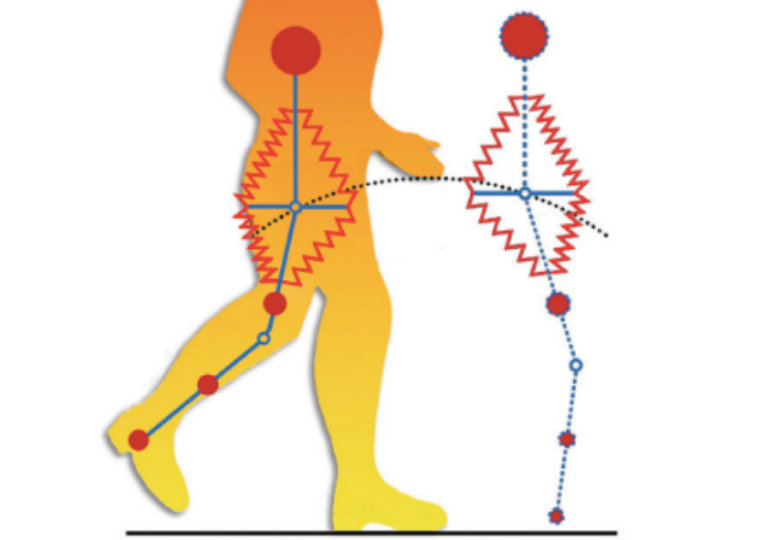
The high stiffness is essential for the locomotion system of the human body. You don’t want your plantar fascia stretched one hundred times more than it is when receiving the body’s weight, do you? The stiff collagen can take a lot of force and store a lot of energy while changing its shape just a little. The source of the misunderstanding is the wonderfully unobtrusive nature way in which collagenous tissue does its job. Collagen is to the body what steel is to technology, and both are the most used materials for the purpose of stability in their respective fields. If you still have any doubts about that, you can try building a suspension bridge with rubber ropes.
It is no wonder that the collagenous tissue of animals was also the preferred material in pre-industrial technology, when elastic material with great stiffness was needed for things like catapults, arch-bow strings, tennis rackets, violins, drum skins, parts of the Zeppelin, and even for condoms.
Second:
The general nomenclature we have for high-tensile, elastic, collagenous tissues rarely indicates accurately their biomechanical function. There are tendons, aponeuroses, fasciae, ligaments, retinaculae, septa, membrana, joint capsules, and many others. However, the sharp distinctions made among these collagenous tissues stem from the dissection of corpses, so there is a lack of understanding about their common function. In fact, the only clear borders between them are those made by the anatomist’s knife.
Two examples:
Aponeuroses are flattened tendons … Fasciae are aponeurotic laminae – early anatomist Henry Gray.3 ‘Fascia’ may be an inappropriate classification for the lumbodorsal fascia because it blends medially with vertebral ligaments and forms aponeurotic attachments for the transversus abdominis and latissimus dorsi muscles, so might also be considered ligamentous or tendinous Priscilla Barker, physiotherapist.4
This nomenclature often tempts biomechanical researchers to consider only tendons while ignoring fascia. Consequently, although it means taking quite a big step away from the established tradition, we would like to support the suggestion of Thomas Findley and Robert Schleip that the term “fascia” be used as a group name “for all kinds of high-tensile, collagenous tissues that have a function in the musculo-skeletal framework.”5
This suggestion was made at the two international conferences on fascia research in 2007 and 2009. (Interestingly, although these conferences were each explicitly named “Fascia Research Congress,” they featured topics on tendons, ligaments, and other tissues.) This naming suggestion was hotly debated because typical examples of tendons and fascia seem to show very different structures when observed under a microscope. Nevertheless, as we are concerned in this chapter with the biomechanical function of fascia, we will use the term fascia as a group name, as defined above, from here forward.
Third:
We would like to address those practitioners of complementary medicine who claim to work only with the elite tissue “fascia,” despising “mundane” muscles. For example, when one of the authors was sharing a practice with another Rolfer, he was not allowed to have dumbbells visibly lying around. By spurning muscle work, practitioners unintentionally make a distinction between tendons and fascia – causing them to work with only one and ignore the other. In addition, we feel such practitioners are missing a real understanding of the human body structure. There is not a single fascia in an awake body that is not exposed to a pull by certain muscles. In our opinion, fascia and muscles must skillfully work together in any accurate representation of the human body.
About the authors

Many years ago I did my doctorate on a topic in semiconductor physics. I have been working in my own Rolfing practice since 1994 (mainly in Berlin, but also partly in the USA and Brazil). I have been a Certified Advanced Rolfer, Rolfing Movement Teacher and Rolfing Mentor since 1999. I have also completed various training courses in psychotherapy (mainly Gestalt and analytical body therapy) and physiotherapy (mainly spiral dynamics). I am licensed as a naturopath. (HeilprG , BA Berlin Hohenschönhausen February 18, 1999, Health Department Berlin-Kreuzberg) In the Fascia Research Project at the University of Ulm (Division of Neurophysiology), I am working as a research assistant on the research of the biomechanical properties of collagenous connective tissue. In sideline jobs I work as a supervisor with social workers, psychologists and doctors in psychosomatic and addiction clinics in Brandenburg and Saxony and develop algorithms for the production of a Stuttgart car manufacturer in a team of engineers. I could formulate my credo for the Rolfing work as follows: “I want the clients to perceive their body as light, graceful, stable and flexible and to enjoy it as much as they do with a valuable musical instrument.” www.rolfing.berlin

Kai Hodeck earned his doctorate in the physics of semiconductor quantum structures at the Berlin University of Technology. Later, his research interests shifted toward biological systems. Today, Hodeck works as a scientist at the Helmholtz Research Center for Materials and Energy, with a focus on thephysics of water in biological systems. He is also a member of the Fascia Research Project team at Ulm University, with a Rolfing® practice in Berlin. Hodeck’s lifelong passion for movement and sports has allowed him to compete in judo, water polo, and dancing. For more than 10 years, he practiced and taught martial arts intensively. This led Hodeck to explore yoga, Feldenkrais®, and, eventually, Rolfing. For more information on the Fascial Research Project atUlm University, Germany, visit www.fasciaresearch.de
References
- Anderson, C.V., & Deban, S.M. (2010). Ballistic tongue projection in chameleons maintains high performance at low temperature,” PNAS, 107(12), 5495-5499. doi:10.1073/pnas.0910778107 Figure 26: Adjo Zorn, walking in Berlin
- Bull, H.B. (1957). Protein structure and elasticity. In J.W. Remington (Ed.), Tissue Elasticity; papers arising from a conference held at Dartmouth College, Hanover, New Hampshire, September 1-3, 1995 (pp. 33-42). Washington, DC: American Physiological Society.
- Gray, H. (1918). Anatomy of the Human Body. Philadelphia, PA: Lea & Febiger.
- Barker, P.J. (2005). Applied anatomy and biomechanics of the lumbar fasciae: implications for lumbopelvic control. (Doctoral dissertation). University of Melbourne, Australia.
- Findley, T.W., & Schleip, R. (2009). Introduction. In P.A. Huijing, A.P. Hollander, T.W. Findley, & R. Schleip (Eds.), Fascia Research II: Basic Science and Implications for Conventional and Complementary Health Care (pp. 2-12). München, Germany: Elsevier Urban & Fischer.
On sale this week only!
Save 25% off the Art of MAT course!
Take an inside look at Myoskeletal Alignment Techniques in action. Follow along with Erik Dalton as he uses MAT techniques to treat real people with real problems. Click the button below for more information and to purchase the course for CE hours and a certificate of completion to display in your office. BONUS: When you purchase the home study course, receive the eCourse for free!
Save 25% this week only. Offer expires May 31st!