Although some are optimistic about the future of stem cell therapy, Murray’s orthopedic surgeon, the legendary Dr. John O’Donnell, believes his only hope for relieving the sharp groin pain is hip resurfacing or a total replacement. “It’s like the brake linings of your car, if you rag them too hard, they wear out earlier; particularly if the hip has suffered previous injury.” In Murray’s case, his degenerative joint disease resulted in a damaged humeral head, loss of joint space, and osteophyte formation. Over time, the repetitive grinding of the femur on the rim of the acetabulum has also caused femoroacetabular impingement syndrome (FAI) and accompanying labral damage (Fig. 2). Although Dr. O’Donnell diagnosed Murray with hip osteoarthritis, I will be referring to the condition as osteoarthrosis (OA) since there is little solid research confirming an inflammatory process in cases of “wear-and-tear” degenerative joint disease.
Primary and Secondary Osteoarthrosis
Let’s look at the two types of osteoarthrosis: primary and secondary. In primary OA the initiating factor is unknown yet it’s commonly seen in weight-bearing joints of women in their 50’s and 60’s. Conversely, in secondary OA, the factor or event is known. For example, in Andy Murray’s case, repetitive movements, recurring injuries, abnormal joint movements, and excessive femoroacetabular loading during his teenage growth spurts are suspected causes. According to research conducted by Abbott et al, a number of manual therapy modalities has been shown to be successful in treating subjects with mild to moderate hip OA.1 These include soft tissue and stretching techniques, articulation maneuvers, and manipulation. Given the close kinetic link between the hips, lumbar spine, sacroiliac, and peripheral joints, it’s best to approach osteoarthrosis from a global viewpoint… that’s one of the goals of Myoskeletal Alignment Techniques (MAT).

How MAT Can Help
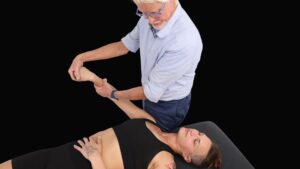
When clients present with reactive muscle guarding in combination with painful femoroacetabular joint restriction, I’ve found greater success by combining MAT with a specifically applied exercise program. I believe that MAT is a great preparation for exercise therapy due to its effect on pain modulation, joint limitations, and muscle hypertonicity. Because MAT techniques use graded exposure stretching and gently articular mobilization to optimize joint lubrication and reduce neuromuscular tone, it’s the perfect combo for those suffering mild to moderate hip osteoarthrosis. Here’s an example of a simple, but effective femoroacetabular MAT routine for clients presenting with his osteoarthrosis pain and/or limited functional mobility.
Hip mobilization for FAI
GOAL: Treating Femoroacetabular Syndrome
LANDMARK: Legs, knees and hips
ACTION:
Step 1:
- Therapist’s right arm snakes on the inside of client’s flexed knee and braces on his own arm
- Therapist’s left hand contacts client’s right thigh
- Therapist distracts and internally rotates client’s femur to barrier and client is asked to adduct the foot against therapist’s resistance to a count of five and relax
- Therapist increases client’s internal femoral rotation restriction by repeating 3 to 5 times
Step 2:
- Next the therapist flexes client’s hip toward her ipsilateral armpit to assess and treat her hip flexion restriction
- Client is asked to gently push her knee into therapist’s body to a count of five and relax and therapist takes her hip to her next restrictive barrier
- Repeat 3 to 5 times
Step 3:
Therapist repeats the same maneuver except this time the line of drive is toward her contralateral armpit
Step 4:
- Therapist pulls client’s left knee toward him and crosses her right foot over so that it contacts the therapy table on the lateral side of her left leg
- Therapist’s right hand contacts client’s right knee and his left hand braces at the client’s right ASIS
- Client is asked to gently push her knee against therapist’s resistance to a count of five and relax and therapist takes her hip to the next adduction barrier
- Repeat 3 to 5 times
1. J.H. Abbott, M.C. Robertson, C. Chapple, D. Pinto, A.A. Wright, S. Leon de la Barra,et al.Manual therapy, exercise therapy, or both, in addition to usual care, for osteoarthritis of the hip or knee: a randomized controlled trial.
On sale this week only!
Save 25% off the Art of MAT course!
Take an inside look at Myoskeletal Alignment Techniques in action. Follow along with Erik Dalton as he uses MAT techniques to treat real people with real problems. Click the button below for more information and to purchase the course for CE hours and a certificate of completion to display in your office. BONUS: When you purchase the home study course, receive the eCourse for free!
Save 25% this week only. Offer expires May 31st!