Median nerve entrapment syndrome
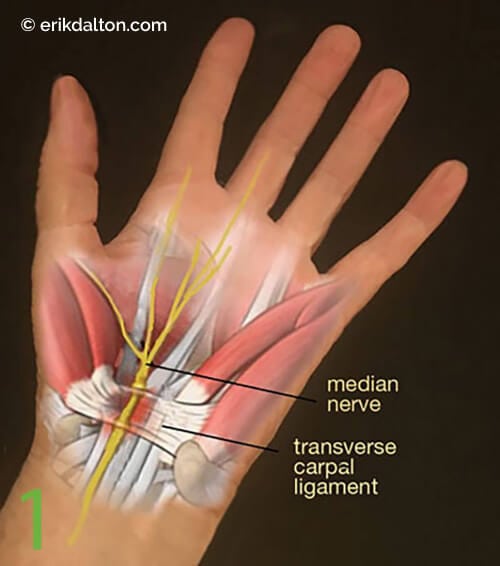
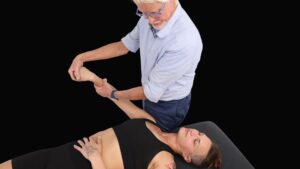
Artists, bodyworkers, computer programmers, and writers are among those who suffer from overuse syndromes such as carpal tunnel syndrome (CTS) (Image 1.). Although most of us have developed hands-on skills for relieving median nerve compression as it passes under the transverse carpal ligament, I believe the treatment can be enhanced by adding simple nerve and joint gliding techniques to your regular routine. This helps reduce inflammation that arises as tendon and nerve sheaths glide across rigid carpal bones.
A 2015 study published in The Journal of Pain reported physical manual therapies that included central nervous system desensitization maneuvers were effective in improving CTS pain.1 By restoring proper carpal joint positioning, massage helps lower intra-tunnel pressure and boosts median nerve glide. I’ve found that gentle carpal bone stretching techniques facilitates longitudinal nerve excursion and reduces protective guarding in the arm flexor muscles. To test this hypothesis, let’s first assess and correct the most common carpal bone fixation (the lunate) and then get the median nerve gliding.
Addressing Lunate-Triquetrum-Scaphoid Mobility
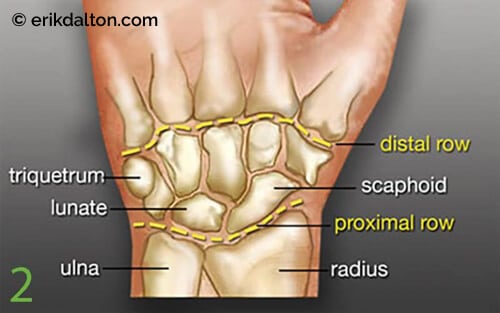
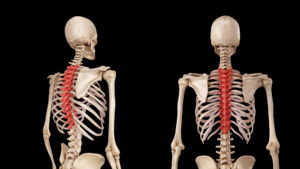
Of the eight carpal bones, the lunate is notoriously the most problematic. It’s prone to sticking (Image 2.), and researchers have discovered that during falls or motor vehicle accidents with the hand outstretched, the lunate can dislocate, compress the flexor tendons, and occlude the median nerve.2 Several orthopedic tests are beneficial in identifying motion-restricted wrist and hand joints, but let’s focus on a single neurological exam I’ve found effective.
To begin, ask the client to touch the tip of the fourth digit to the thumb and hold firmly, as you moderately attempt to pull these fingers apart, testing the non-affected hand first. Weakness in the ring finger’s opposition to the thumb usually indicates a triquetrum-lunate fixation. Conversely, weakness when testing the third digit’s opposition to the thumb incriminates the lunate-scaphoid joint. The osteoligamentous stretches shown in Images 3 and Image 4 are designed to correct lunate fixations. I encourage you to add these stretches to your current CTS repertoire.
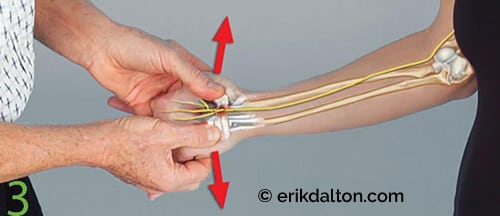
Image 3. Osteoligamentous stretches to correct lunate fixations
- With the client’s elbow and wrist slightly flexed (palm up), the fingers of the therapist and client interlace.
- The therapist’s thumbs glide superiorly until they bump into the radius and ulna bones, and move slightly medially to contact the triquetrum and scaphoid.
- Holding mild sustained pressure, the client palmar-flexes the wrist against the therapist’s resistance to a count of five and then relaxes.
- The therapist gently extends the client’s wrist while his thumbs spread the triquetrum and scaphoid laterally to open the tunnel and drag the lunate away from the median nerve.
- Repeat 3–5 times.
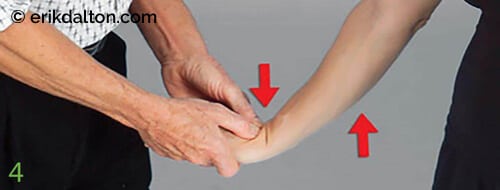
Image 4. Osteoligamentous stretches to correct lunate fixations
- To create space between the proximal carpal row and the radius/ulna, the therapist extends and gently tractions the elbow and wrist up to, but not entering, the painful barrier.
- With the therapist’s thumbs positioned on the proximal carpal row, the client slowly palmar-flexes the wrist against the therapist’s resistance to a count of five and then relaxes.
- The therapist’s fingers extend the wrist and traction the arm with the intent of spreading the tunnel, gliding the carpals free of the radius/ulna, and stretching the median nerve.
- Repeat 3–5 times, and then retest the ability of the third and fourth digits to oppose the thumb.
Restoring CTS Nerve Glide
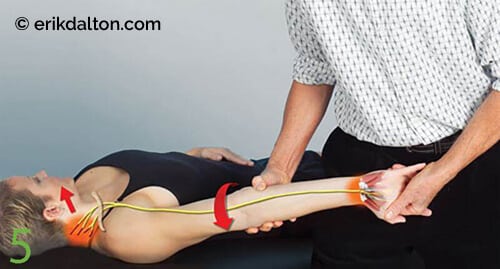
Image 5. Neural Glide Routine
- The therapist abducts and externally rotates the client’s arm to 90/90 position.
- The client is asked to depress and retract her scapula and hold it there.
- The therapist supinates the client’s arm and extends the fingers and wrist.
- The therapist slowly begins to extend the client’s elbow until discomfort occurs.
- The client left side-bends her head as the therapist adducts her arm to reduce stretch of the nerve.
- As she brings her head back to neutral, the therapist again extends and externally rotates her arm, wrist, fingers, and elbow.
- Slowly repeat the back-and-forth nerve flossing until symptoms improve.
Summary
References
- C. Fernández-de-Las Peñas et al., “Manual Physical Therapy Versus Surgery for Carpal Tunnel Syndrome: A Randomized Parallel-Group Trial,” The Journal of Pain 16, no. 11 (November 2015): 1087–94.
- Eren Cansü et al., “Neglected Lunate Dislocation Presenting as Carpal Tunnel Syndrome,” Case Reports in Plastic Surgery and Hand Surgery 2, no. 1 (January 2015): 22–24, doi:10.3109/23320885.2014.993397.
On sale this week only!
Save 25% off the Dynamic Lower Body Course!
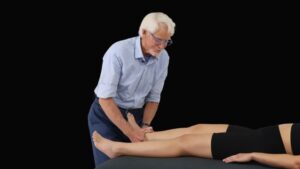
Most lower body pain doesn’t start where it shows up. In the Dynamic Lower Body course, you’ll learn how to assess and treat the real drivers behind low back, hip, and leg dysfunction using a clear, systematic MAT approach. From sciatica and SI joint issues to knee pain and plantar fasciitis, you’ll connect the dots across the entire kinetic chain. If you’re ready to stop chasing symptoms and start delivering consistent, lasting results, this course gives you the framework to do it. Save 25% this week only. Sale ends Sunday, May 24th.
BONUS: When you purchase the home study course, receive the eCourse for free!